What is the purpose of the Medication Count Sheet?
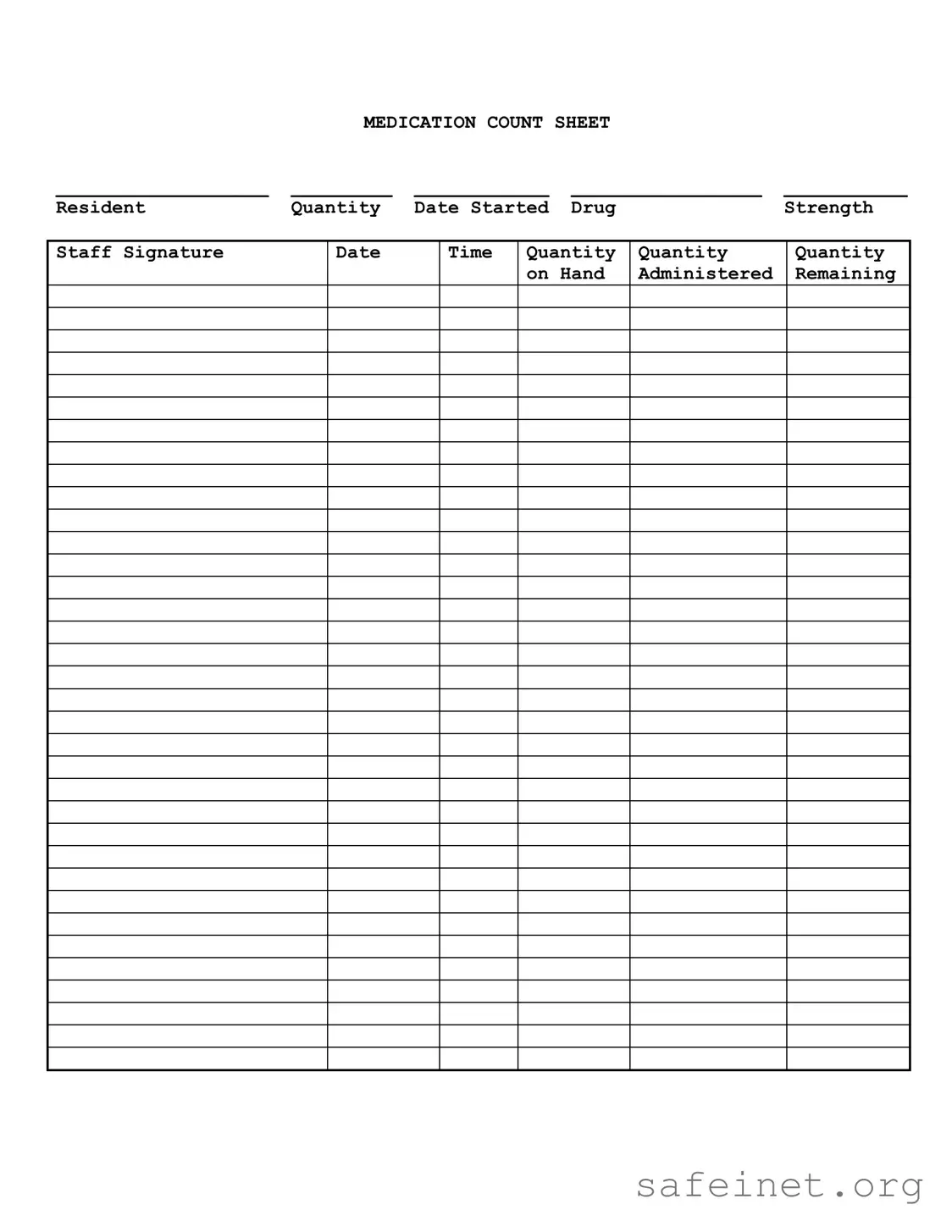
The Medication Count Sheet is designed to help healthcare providers track the administration and inventory of medications for residents. It ensures that accurate records are maintained, which is crucial for patient safety and compliance with regulations. By documenting the quantity of medication on hand, administered, and remaining, staff can prevent errors and ensure that residents receive their prescribed treatments on time.
What information is required on the Medication Count Sheet?
The Medication Count Sheet requires several key pieces of information. This includes the resident's name, the quantity of medication, the date the medication was started, the drug strength, and the staff signature. Additionally, it is important to record the date and time of administration, along with the quantities administered and remaining. This comprehensive data helps maintain an accurate medication log.
Who is responsible for filling out the Medication Count Sheet?
Staff members who are authorized to administer medications are responsible for completing the Medication Count Sheet. This typically includes nurses and certified nursing assistants. It is essential that the staff member who administers the medication also records the necessary details on the form to ensure accountability and accuracy in medication management.
How often should the Medication Count Sheet be updated?
The Medication Count Sheet should be updated each time medication is administered. This means that every dose given must be recorded immediately to reflect the current inventory accurately. Additionally, regular audits may be conducted to verify the information on the sheet against the actual medication supply, ensuring consistency and accuracy over time.
What should be done if there is a discrepancy in the medication count?
If a discrepancy is found in the medication count, it is crucial to report it immediately to a supervisor or the designated medication management personnel. Investigating the cause of the discrepancy should be a priority, as it could indicate a potential error in administration or record-keeping. Proper procedures should be followed to ensure that the issue is resolved and that patient safety is maintained.
Can the Medication Count Sheet be used for different types of medications?
Yes, the Medication Count Sheet can be used for various types of medications, including oral medications, injections, and topical treatments. It is a versatile tool that can accommodate different drug forms, as long as the necessary details are recorded. This adaptability makes it a valuable resource in various healthcare settings.
Is training required for staff to use the Medication Count Sheet?
Yes, staff should receive training on how to properly use the Medication Count Sheet. This training should cover the importance of accurate record-keeping, how to fill out the sheet correctly, and the protocols for reporting discrepancies. Ensuring that all staff members are knowledgeable about the process is essential for maintaining high standards of patient care.
What should be done with the Medication Count Sheet after it is filled out?
Once the Medication Count Sheet is filled out, it should be securely stored in accordance with the facility's policies on record retention. This ensures that the information remains accessible for audits and reviews while also protecting patient privacy. Regular reviews of these sheets can also help identify patterns or areas for improvement in medication management practices.