What is the purpose of the CNA Shower Sheets form?
The CNA Shower Sheets form is designed to help Certified Nursing Assistants (CNAs) conduct a thorough visual assessment of a resident’s skin during showering. This form enables CNAs to document any abnormalities, such as bruising, rashes, or lesions, and ensures that these findings are communicated to the charge nurse and the Director of Nursing (DON) for further evaluation. By using this form, CNAs play a crucial role in monitoring residents' skin health and preventing potential complications.
What types of skin abnormalities should I look for during the assessment?
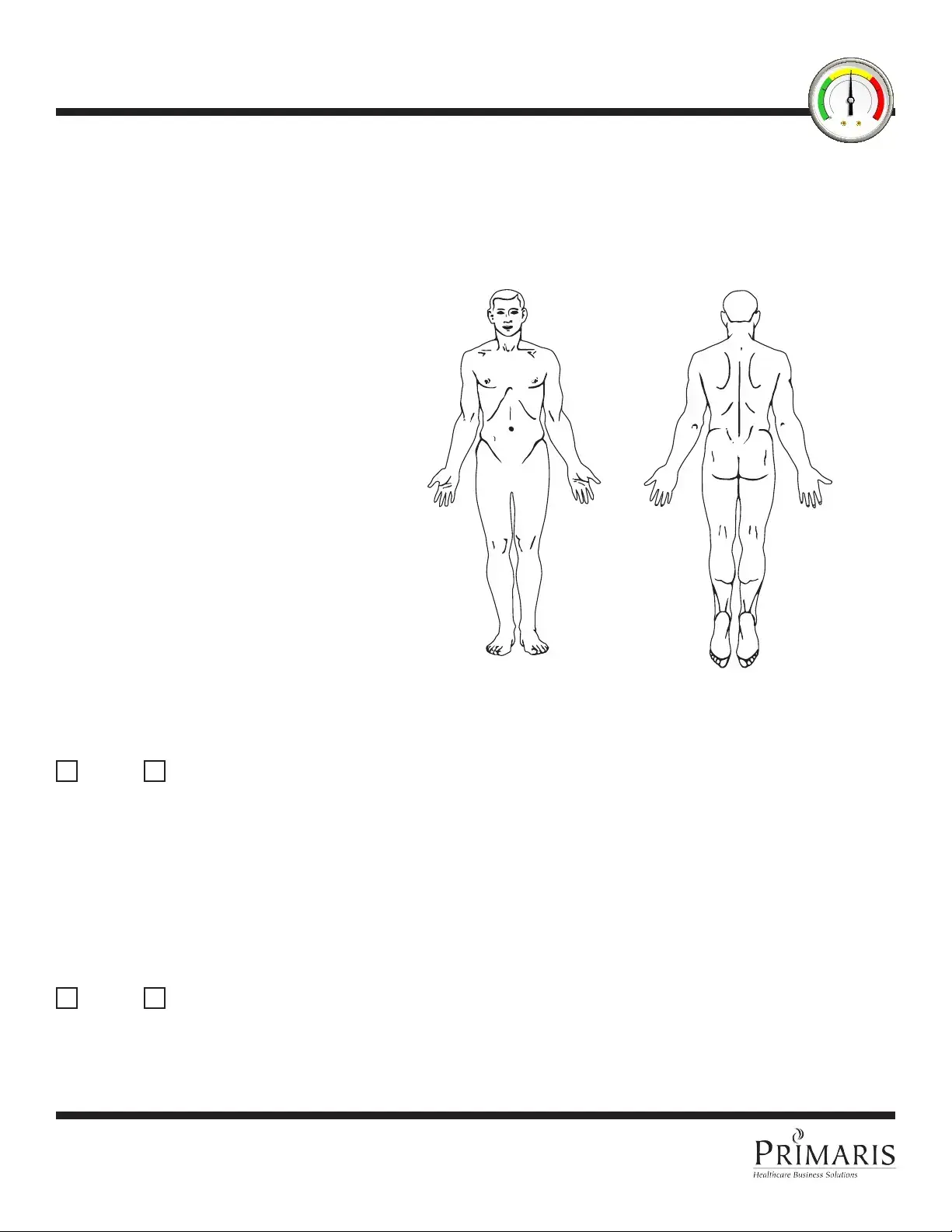
During the shower assessment, CNAs should be vigilant for various skin abnormalities. Common issues to note include bruising, skin tears, rashes, swelling, dryness, and lesions. Additionally, pay attention to soft heels, decubitus ulcers, blisters, scratches, and any unusual skin color or temperature. Each of these conditions can indicate underlying health concerns that may require immediate attention. The form provides a body chart for CNAs to accurately mark and describe the location of these abnormalities.
What should I do if I find an abnormality on a resident's skin?
If you observe any abnormal skin conditions during the assessment, it is essential to report them to the charge nurse right away. The charge nurse will then evaluate the situation and decide on the necessary interventions. Afterward, the findings should be documented on the CNA Shower Sheets form, and any significant issues should be forwarded to the DON for further review. Prompt reporting helps ensure that residents receive the care they need in a timely manner.
How do I document my findings on the CNA Shower Sheets form?
To document your findings, start by filling out the resident's name and the date at the top of the form. As you conduct your visual assessment, use the provided body chart to graphically represent the location of any abnormalities. Next, describe each finding in the designated sections, noting the type of abnormality and any other relevant details. Don’t forget to sign and date the form after completing your assessment. Clear documentation is key to effective communication within the care team.
Is there anything else I need to do after completing the form?
Yes, after you complete the CNA Shower Sheets form, make sure to check if the resident needs their toenails cut, as indicated on the form. Once you have filled out all necessary sections, pass the form to the charge nurse for their assessment and signature. Finally, ensure that the form is forwarded to the DON if required. This process helps maintain a comprehensive record of the resident's skin health and ensures that all team members are informed of any concerns.